Migraine: East vs West
Migraine is a common, often disabling primary headache disorder characterized by recurrent attacks of moderate to severe head pain with sensory hypersensitivity (photophobia, phonophobia), nausea, and
Promising research with growing clinical support from multiple studies
Tension-type headache (TTH) is the most common primary headache worldwide, typically described as a dull, pressing, band-like pain on both sides of the head, often with neck or scalp tenderness and without the nausea, vomiting, or disabling sensitivity to light and sound characteristic of migraine. From a western biomedical perspective, episodic TTH is diagnosed clinically using criteria from the International Classification of Headache Disorders (ICHD-3), which emphasize headache frequency, duration (30 minutes to 7 days), and features (bilateral, pressing/tightening quality, mild to moderate intensity, not aggravated by routine activity). Triggers often include stress, prolonged screen time or poor ergonomics, jaw clenching, sleep disruption, dehydration, and missed meals. Pathophysiology appears to involve pericranial muscle tenderness and central sensitization—meaning the nervous system becomes more responsive to pain over time, particularly in chronic TTH. Traditional Chinese Medicine (TCM) frames similar symptoms as patterns such as Liver Qi stagnation, Qi and Blood deficiency, or external “wind” invasion leading to meridian imbalance along the Gallbladder, Bladder, and Liver channels. Neck and scalp tension may reflect obstructed flow of Qi and Blood; stress exacerbates Liver Qi stagnation, and overwork or poor diet weakens Spleen Qi, contributing to recurrent head pain. When people ask about alternatives for TTH, they often mean non-drug approaches. In western practice, several non-pharmacologic options have supportive evidence. Physical therapy and manual therapy target tight neck and shoulder muscles, posture, and scapular stabilization; these may include myofascial release and trigger-point techniques. Patients with palpable pericranial tenderness, forward-head posture, or computer-based jobs often respond well. Massage therapy can reduce muscle tension and promote relaxation; evidence suggests short-term relief with minimal risks such as transient sore
This content is for informational purposes only and does not constitute medical advice. Always consult a qualified healthcare provider before starting, stopping, or changing any supplement or medication regimen.
Clinical diagnosis guided by ICHD-3 criteria: bilateral, pressing/tightening head pain of mild to moderate intensity, not worsened by routine activity, lasting 30 minutes to 7 days; no prominent nausea or vomiting and at most one of photophobia or phonophobia. Evaluation includes history of triggers (stress, posture, bruxism), medication use (to rule out medication-overuse headache), and targeted exam for pericranial muscle tenderness and neck/jaw dysfunction. Neuroimaging is not routinely indicated unless red flags are present (sudden severe onset, new neurological deficits, fever, trauma, cancer/immunosuppression, age >50 with new headache).
- Many non-pharmacologic therapies require consistent practice and access to trained clinicians; insurance coverage varies. - Analgesics can help acutely but frequent use risks medication-overuse headache and gastrointestinal or renal adverse effects with NSAIDs. - Tricyclic antidepressants can reduce headache frequency but may cause dry mouth, drowsiness, weight gain, and other side effects. - Spinal manipulation evidence for TTH is mixed; rare but serious complications have been reported with high-velocity cervical techniques. - Not all patients respond; central sensitization and psychosocial factors can maintain headaches despite good technique.
Sources
TCM attributes tension-type patterns to stagnation of Liver Qi from stress, Qi and Blood deficiency from overwork or diet, or external wind obstructing channels along the head and neck. Treatment aims to restore the smooth flow of Qi and Blood, disperse wind, and relieve meridian blockages.
Manual stimulation of acupuncture points is used to move Qi and relieve local muscle tension without needles. It is commonly taught for LI4, GB20, and Taiyang to manage episodic TTH and stress.
Gentle movement, breath regulation, and focused attention are used to harmonize Qi, downshift sympathetic arousal, and improve posture and neck-shoulder mobility—factors implicated in TTH.
Headaches may relate to aggravated Vata (wind) or Pitta (heat) with muscular tension and stress. Care aims to pacify doshic imbalance, calm the nervous system, and improve digestion and sleep.
Sources
Integrative care often combines a biomedical evaluation (to confirm tension-type pattern and screen for red flags) with a personalized mix of behavioral, physical, and traditional therapies. Practical pathways include: pairing CBT or relaxation training with acupuncture to target both central sensitization and muscle/meridian tension; coordinating physical therapy for posture and scapular strength with TCM cupping or tui na on tight cervical/shoulder musculature; and adding qigong or tai chi as ongoing self-care to maintain gains. Some clinics offer biofeedback alongside acupuncture—early studies suggest additive benefits on stress reactivity and headache days, but high-quality trials of combined approaches are still limited. Safety and interactions: acupuncture and cupping carry low risk when performed by trained professionals, but easy bruising, anticoagulant therapy, or bleeding disorders warrant caution. Herbal formulas can interact with medications: herbs like chuan xiong (Ligusticum chuanxiong), angelica (Dang Gui), or danshen (Salvia miltiorrhiza) may have antiplatelet effects; licorice (Glycyrrhiza) can raise blood pressure and lower potassium; quality control varies by manufacturer. Tricyclic antidepressants (e.g., amitriptyline) and certain supplements or herbs affecting serotonin or norepinephrine could theoretically interact; pharmacists or knowledgeable clinicians can help review combinations. Contraindications and red flags requiring conventional evaluation include: sudden “worst headache of life,” new neurological deficits (weakness, speech or vision changes), fever/neck stiffness, head trauma, progressive pattern change, onset after age 50, cancer or immunosuppression, or headaches triggered by exertion/sexual activity. Frequent analgesic use (most days per week) increases risk of medication-overuse headache; structured tapering plans are best handled with clinical guidance. Cost, access, and outcomes: CBT/biofeedback and PT often have moderate-to-strong evidence and durable benefits when skills are maintained. Acupuncture has moderate-quality evidence for reducing headache frequency with generally favorable safety and patient satisfaction. Massage, acupressure, tai chi/qigong, and spinal manipulation show emerging-to-mixed evidence; they may help selected patients, especially those with prominent muscle tension or stress triggers. Availability, insurance coverage, and out-of-pocket costs vary widely. Tracking a headache diary, practicing daily relaxation or breathwork, and aligning posture/ergonomics can make any approach more effective. Consult your healthcare provider before making changes to your health regimen.

The Trigger Point Therapy Workbook, Third Edition, has made a huge impact among health professionals and the public alike, becoming an overnight classic in the field of pain relief. This edition inclu

Doctor's Best High Absorption Magnesium Glycinate Lysinate Supplement for Sleep Support - Chelated Magnesium Capsules for Women & Men, 105 mg per Serving, Calm Support, Vegan - 120 Veg Caps
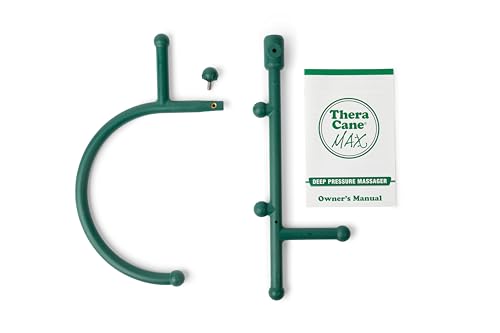
<strong>Amazingly simple yet effective self-massager makes it easy to apply pain-relieving deep compression directly to hard, knotted "trigger points" anywhere they occur</strong>. Break up
Migraine is a common, often disabling primary headache disorder characterized by recurrent attacks of moderate to severe head pain with sensory hypersensitivity (photophobia, phonophobia), nausea, and
Holistic Treatment for Temporomandibular Joint Disorder (TMJ). Temporomandibular disorders (TMD, often called TMJ) involve the jaw joint, chewing muscles, and related structures. They commonly present with jaw pain, limited or painful opening, clicking or popping, and headaches or ear symptoms. Comparing Western and Eastern perspectives is useful because each t
Natural Remedies for Headaches: Evidence‑Based Herbs, Supplements & Self‑Care. If you’re searching for natural remedies for headaches, you’re not alone. Many people want options that ease pain, reduce frequency, and feel gentler than daily medications. This guide brings together western research and time‑tested eastern practices, clearly labeling the strength of evidence behin
Migraine and Chiropractic Care. Migraines are a common neurologic disorder marked by recurrent, often disabling headache attacks with sensitivity to light and sound, nausea, and sometimes aura. Many people with migraine also report neck pain and stiffness before or during attacks. This neck–head connection has a plausible biologic
Migraine and Triptans. Migraines are disabling headaches driven by abnormal brain excitability and sensitized pain pathways. Triptans are a family of medicines that target key steps in this process by activating specific serotonin (5‑HT) receptors on cranial nerves and blood vessels. They are indicated for acute treatment
Temporomandibular Joint Disorder (TMJ/TMD). Temporomandibular joint disorders (TMJ/TMD) encompass pain and dysfunction involving the jaw joint, chewing muscles, and related structures. Estimates vary, but roughly 5–10% of adults experience clinically significant symptoms at any time, with women affected more often. Causes are multifactorial:
Health Disclaimer
This content is for informational purposes only and does not constitute medical advice. Always consult a qualified healthcare provider before starting, stopping, or changing any supplement or medication regimen.