Traditional Chinese Medicine
Traditional Chinese Medicine (TCM): Overview
Traditional Chinese Medicine (TCM) is a broad medical system that developed over thousands of years in China and East Asia. Rather than focusing only on isolated symptoms or organ pathology, TCM traditionally interprets health as a dynamic state of balance within the body and between the body and its environment. Its core concepts include qi (often described as vital energy or functional activity), yin and yang balance, the Five Phases/Elements, and the interconnected function of organ systems understood through a distinct theoretical framework. TCM is not a single therapy, but a modality umbrella that includes practices such as acupuncture, herbal medicine, moxibustion, cupping, tui na massage, tai chi, and qigong, along with individualized dietary and lifestyle guidance.
TCM remains one of the most widely used traditional medical systems in the world. It is practiced extensively in China and has become increasingly integrated, adapted, or studied in many other countries. In modern healthcare settings, TCM may be used as a complementary approach alongside conventional medicine, particularly for chronic pain, functional disorders, stress-related complaints, recovery support, and general well-being. At the same time, its use varies considerably depending on regulation, practitioner training, product quality standards, and the availability of evidence for specific therapies.
A defining feature of TCM is its emphasis on pattern differentiation. Instead of assigning treatment based solely on a biomedical diagnosis, practitioners traditionally assess patterns such as deficiency, excess, heat, cold, dampness, stagnation, or disharmony affecting particular functional networks. Two people with the same conventional diagnosis may therefore receive different TCM assessments and different therapeutic approaches. This individualized framework is central to TCM practice, but it can also make the modality more difficult to study using standard biomedical research designs.
In contemporary health discussions, TCM occupies a complex position. Some individual TCM therapies—especially acupuncture for certain pain conditions and mind-body practices such as tai chi and qigong—have been studied extensively and are included in some clinical guidelines. Other areas, particularly multi-herb formulas individualized to a TCM pattern, remain harder to evaluate and often have more mixed or limited evidence. Quality control, herb-drug interactions, safety monitoring, and the role of TCM within integrative care are therefore major topics in both research and policy.
Medical Perspectives
Two Ways of Seeing Health

Western
scientific · clinical
Western medicine applies science, technology, and clinical experience to treat symptoms through testing, diagnosis, and targeted intervention.

Eastern
traditional · alternative
Eastern medicine focuses on treating the body naturally by applying traditional knowledge practiced for thousands of years, emphasizing balance and whole-person wellness.
Gold Bamboo presents both perspectives side-by-side so you can make informed decisions. We don't advocate for one over the other — your health choices are yours.
Western Medicine Perspective
Western / Conventional Medicine Perspective
From a conventional medical standpoint, TCM is understood as a heterogeneous group of interventions rather than a single scientifically unified treatment. Western medicine typically evaluates TCM components separately—for example, acupuncture, herbal products, tai chi, or cupping—using clinical trials, systematic reviews, pharmacology, physiology, and safety surveillance. This approach does not validate traditional explanatory models such as qi or meridians in the same way they are used within TCM theory, but it does examine whether particular practices produce measurable health effects, how large those effects are, and in which patient populations they may be relevant.
Among TCM-related modalities, acupuncture has the strongest research base in conventional literature, especially for some forms of chronic pain, including low back pain, osteoarthritis-related pain, neck pain, and headache disorders. Studies and meta-analyses suggest that benefits may exist for selected conditions, although debate continues about mechanisms, effect size, sham controls, and how much benefit is specific to needling versus contextual or nonspecific therapeutic effects. Tai chi and qigong are also viewed favorably in many conventional settings as low-impact movement and mind-body practices associated with improvements in balance, mobility, stress regulation, and some chronic disease-related quality-of-life outcomes.
Conventional medicine is generally more cautious regarding TCM herbal medicine, not because plant-based therapies are inherently dismissed, but because concerns often center on standardization, contamination, adulteration, variable dosing, herb-drug interactions, and inconsistent trial quality. Some herbs and formulas have been studied and show promise in specific contexts, while others lack robust evidence or raise safety concerns, including potential liver toxicity, kidney injury, heavy metal contamination, or the presence of undeclared pharmaceuticals in poorly regulated products. For this reason, modern biomedical evaluation places significant emphasis on manufacturing standards, toxicology, and communication between patients and healthcare professionals.
In integrative medicine, TCM is often framed as a complementary modality that may have value for symptom management, supportive care, rehabilitation, and patient-centered chronic disease management when delivered by appropriately trained professionals. Conventional clinicians generally distinguish between evidence-supported use for defined symptoms and broader traditional claims that remain difficult to confirm scientifically. Consultation with qualified healthcare providers is considered especially important when TCM is used alongside prescription medications, during pregnancy, or in the context of serious medical illness.
Eastern & Traditional Perspective
Eastern / Traditional Medicine Perspective
Within Traditional Chinese Medicine itself, health is traditionally understood as the harmonious flow of qi, blood, yin, yang, and body fluids, coordinated through organ systems and meridian networks. Illness is not seen solely as a localized defect but as a disturbance in the body’s overall pattern of balance. Diagnosis traditionally involves methods such as observation, pulse assessment, tongue examination, inquiry, and palpation, leading to a pattern-based interpretation rather than a disease label alone. Treatment aims to restore balance, regulate functional relationships, and support the body's capacity to recover.
TCM practitioners traditionally use a range of methods depending on the identified pattern. Acupuncture is used to influence meridian function and regulate qi flow; herbal formulas are combined according to classical principles intended to match the individual’s presentation; moxibustion is used to warm or stimulate specific points; cupping and tui na are applied to address stagnation or musculoskeletal complaints; and tai chi and qigong are cultivated to support circulation, breath, posture, and mind-body integration. In traditional practice, these methods are often combined rather than used in isolation.
Other traditional systems sometimes intersect with TCM in philosophy, though they remain distinct medical traditions. Ayurveda, for example, similarly emphasizes constitutional balance, digestion, environment, and individualized care, while naturopathic and East Asian medicine frameworks may incorporate TCM concepts alongside nutrition, botanical medicine, and lifestyle practices. Across these traditions, common themes include prevention, regulation of daily rhythms, attention to digestion and stress, and the idea that chronic illness may reflect systemic imbalance rather than a single isolated cause.
From an eastern and traditional perspective, the significance of TCM lies not only in symptom relief but in its whole-person orientation—addressing physical, emotional, environmental, and behavioral factors together. This systems-based view has contributed to its enduring use. At the same time, many contemporary traditional practitioners also recognize the value of modern diagnostics, emergency care, and collaborative integrative practice, particularly when symptoms may indicate conditions requiring conventional medical evaluation.
Supplements & Products
Recommended Products

The Web That Has No Weaver : Understanding Chinese Medicine: Kaptchuk, Ted J.
Ted J. Kaptchuk ... A Doody’s Core Title for 2024 & 2022! The Web That Has No Weaver is <strong>the classic, comprehensive guide to the theory and practice of Chinese alternative medicine</strong>

Kangzhu 24-Cup Biomagnetic Chinese Cupping Therapy Set
Cupluw Cupping Set, 24 Cups Cupping Kit for Massage Therapy, Chinese Cupping Therapy Set with Magnetics, Professional Vacuum Cupping Set for Cellulite Reduction Muscle Pain Relief with Manual Pump
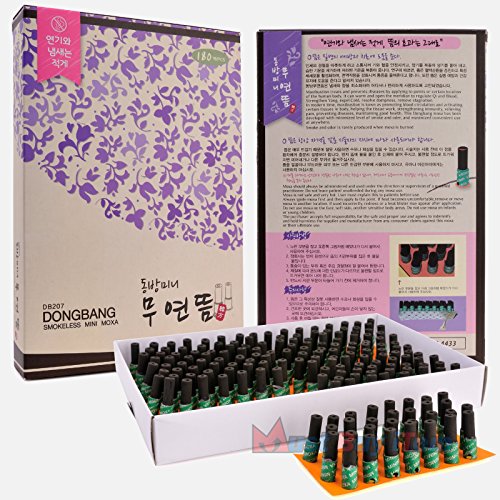
DongBang Acupuncture 100% Wormwood Mugwort Moxibustion Mini Smokeless Moxa Sticks On Cone Roll 1Box 180pcs
Buy DongBang Acupuncture 100% Wormwood Mugwort Moxibustion Mini Smokeless Moxa Sticks On Cone Roll 1Box 180pcs on Amazon.com ✓ FREE SHIPPING on qualified orders
Evidence & Sources
Promising research with growing clinical support from multiple studies
- World Health Organization (WHO) Traditional Medicine Strategy
- National Center for Complementary and Integrative Health (NCCIH)
- JAMA Internal Medicine
- BMJ
- Cochrane Reviews
- Annals of Internal Medicine
- PLOS Medicine
- The Journal of Alternative and Complementary Medicine
This content is for informational purposes only and does not constitute medical advice. Always consult a qualified healthcare provider before starting, stopping, or changing any supplement or medication regimen.

