Myofascial Pain Syndrome
Also known as: Trigger Point Pain, Myofascial Pain
Overview
Myofascial pain syndrome (MPS) is a chronic pain condition characterized by regional muscle pain, localized tenderness, and the presence of myofascial trigger points—hyperirritable spots within taut bands of skeletal muscle or surrounding fascia. Unlike brief post-exercise soreness, MPS often persists over time and may be associated with stiffness, reduced range of motion, referred pain patterns, sleep disturbance, fatigue, and functional limitation. It can affect the neck, shoulders, low back, jaw, pelvis, and other regions, and is commonly discussed alongside posture-related strain, repetitive use, stress, injury, and prolonged immobility.
The condition is clinically important because it sits at the intersection of musculoskeletal medicine, pain science, rehabilitation, and integrative care. People frequently seek information about massage, stretching, physical therapy, dry needling, acupuncture, and fascia-oriented therapies because MPS is often experienced as both a local tissue problem and a nervous-system pain sensitivity issue. It may occur on its own or overlap with tension-type headache, temporomandibular disorders, low back pain, fibromyalgia, and occupational overuse syndromes.
Diagnosis is typically based on history and physical examination, rather than a single definitive lab or imaging test. However, the concept and diagnostic criteria for trigger points have been debated in the medical literature, and researchers do not always agree on how reliably they can be identified between examiners. As a result, MPS is best understood as a real clinical pain presentation with evolving scientific models, rather than a perfectly uniform disease entity.
From a broader health perspective, research suggests that myofascial pain is often influenced by multiple factors at once, including muscle overload, biomechanical strain, stress physiology, sleep quality, mood, central sensitization, and recovery capacity. This multifactorial nature helps explain why conventional and traditional systems alike often describe MPS using multidimensional frameworks and why care discussions commonly involve movement, manual therapies, mind-body approaches, and broader pain management strategies. Anyone with persistent or worsening pain, neurologic symptoms, trauma, fever, unexplained weight loss, or other concerning signs is generally advised to seek evaluation from a qualified healthcare professional.
Medical Perspectives
Two Ways of Seeing Health

Western
scientific · clinical
Western medicine applies science, technology, and clinical experience to treat symptoms through testing, diagnosis, and targeted intervention.

Eastern
traditional · alternative
Eastern medicine focuses on treating the body naturally by applying traditional knowledge practiced for thousands of years, emphasizing balance and whole-person wellness.
Gold Bamboo presents both perspectives side-by-side so you can make informed decisions. We don't advocate for one over the other — your health choices are yours.
Western Medicine Perspective
Western Medicine Perspective
In conventional medicine, myofascial pain syndrome is generally viewed as a regional musculoskeletal pain disorder involving sensitive spots in muscle and fascia, often associated with motor dysfunction, altered muscle activation, and pain referral patterns. Proposed mechanisms include local muscle overload, microtrauma, sustained contraction, ischemia, inflammatory mediators, and changes in the peripheral and central nervous systems that amplify pain. Modern pain science also emphasizes that chronic myofascial pain may reflect more than local tissue tension alone; in some cases it appears to involve central sensitization, where the nervous system becomes more responsive to pain signals.
Assessment typically focuses on symptom pattern, palpation findings, movement limitations, occupational and ergonomic factors, stress, sleep, and exclusion of other causes such as radiculopathy, inflammatory disease, infection, fracture, or systemic illness. Imaging and laboratory testing are not usually diagnostic for MPS itself, though they may be used to rule out competing explanations. Conventional management discussions often include physical therapy, exercise-based rehabilitation, postural and ergonomic modification, trigger point techniques, manual therapy, dry needling, medication options for pain modulation, and education about chronic pain mechanisms. Research indicates some patients improve with multimodal approaches, but outcomes vary, and no single therapy is universally effective.
The evidence base is mixed but substantial enough to support clinical interest. Dry needling, manual therapies, and exercise have been studied for myofascial pain in the neck, shoulder, jaw, and back, with many trials showing short-term symptom improvement; however, methodological quality is variable, and long-term comparative data remain limited. This is one reason mainstream guidelines tend to favor a functional, individualized, and multimodal rehabilitation approach over a single trigger-point-centered explanation.
Eastern & Traditional Perspective
Eastern and Traditional Medicine Perspective
In Traditional Chinese Medicine (TCM), symptoms resembling myofascial pain syndrome are often interpreted through patterns such as Qi and Blood stagnation, obstruction of the channels and collaterals, or invasion of wind-cold-damp in vulnerable tissues. Taut, painful bands and fixed tender spots may be understood as areas where circulation and energetic flow have become constrained. Emotional stress, overwork, poor recovery, and constitutional weakness may also be considered contributing factors. Traditional approaches have commonly included acupuncture, moxibustion, cupping, tui na bodywork, movement practices such as tai chi or qigong, and pattern-based herbal medicine, with the goal of restoring circulation, easing spasm, and supporting overall balance.
In Ayurveda, persistent muscular pain and stiffness may be framed in terms of vata imbalance, impaired tissue nourishment, and obstruction in the body’s channels, sometimes with contributions from accumulated metabolic residue described traditionally as ama. Fascia-like connective tissue relationships may be discussed through concepts involving mamsa dhatu and srotas. Traditional Ayurvedic care has often involved abhyanga oil massage, fomentation, stretching or yoga-based movement, marma-focused bodywork, and individualized herbal formulations, with the broader aim of calming aggravated movement qualities in the body and improving tissue resilience.
In naturopathic and other integrative traditions, myofascial pain is frequently viewed as a manifestation of structural strain plus whole-person stress burden. Sleep quality, inflammation, nervous-system regulation, hydration status, breathing patterns, and physical deconditioning may all be considered relevant. These systems often emphasize that chronic soft-tissue pain is rarely just a local mechanical issue. While traditional frameworks differ from biomedical terminology, they often converge with modern integrative pain care in valuing manual medicine, movement re-education, stress regulation, and individualized assessment. As with conventional care, the quality of evidence varies across modalities, and consultation with appropriately trained practitioners is important.
Supplements & Products
Recommended Products

The Trigger Point Therapy Workbook: Your Self-Treatment Guide for Pain Relief: Davies NCTMB, Clair, Davies CMTPT LMT, Amber, Simons MD, David G.
The Trigger Point Therapy Workbook, Third Edition, has made a huge impact among health professionals and the public alike, becoming an overnight classic in the field of pain relief. This edition inclu
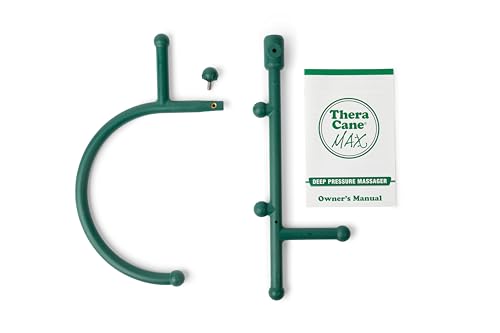
Thera Cane Massager (Green, Single)
<strong>Amazingly simple yet effective self-massager makes it easy to apply pain-relieving deep compression directly to hard, knotted "trigger points" anywhere they occur</strong>. Break up

TriggerPoint GRID Foam Roller for Exercise, Deep Tissue Massage and Muscle Recovery, Original (13-Inch)
The 13-inch GRID X features <strong>extra dense foam for working the tightest muscles</strong>. Purchase of any TriggerPoint GRID foam roller includes free access to an online instructional video libr
Evidence & Sources
Promising research with growing clinical support from multiple studies
- National Center for Complementary and Integrative Health (NCCIH)
- American Academy of Family Physicians
- The Journal of Pain
- Pain
- The Clinical Journal of Pain
- Cochrane Database of Systematic Reviews
- Journal of Bodywork and Movement Therapies
- BMJ
- Mayo Clinic Proceedings
- World Health Organization (WHO)
This content is for informational purposes only and does not constitute medical advice. Always consult a qualified healthcare provider before starting, stopping, or changing any supplement or medication regimen.

