Long COVID
Also known as: Post-COVID Syndrome, Post-Acute Sequelae of COVID-19, PASC
Overview
Long COVID—also called post-COVID condition or post-acute sequelae of SARS-CoV-2 infection (PASC)—describes a constellation of symptoms that persist, recur, or newly appear after the initial phase of COVID-19. Definitions vary somewhat across organizations, but the condition is generally recognized when symptoms continue for weeks to months beyond acute infection and cannot be fully explained by another diagnosis. Commonly reported features include fatigue, exertional intolerance, shortness of breath, cognitive dysfunction (“brain fog”), sleep disturbance, palpitations, dizziness, pain, loss of smell or taste, anxiety, and mood changes.
Long COVID is clinically significant because it can affect multiple organ systems and range from mild but disruptive to profoundly disabling. Research suggests that it occurs after both severe and mild initial infections, including in people who were never hospitalized. Prevalence estimates differ depending on the population studied, viral variant, vaccination status, and definition used, but major public health organizations recognize it as an important ongoing consequence of the pandemic. Its heterogeneity is one reason it remains challenging to study and manage.
Current scientific understanding suggests that Long COVID is not a single disorder, but rather a syndrome with several potential biological drivers. Proposed mechanisms include immune dysregulation, persistent inflammation, autonomic nervous system dysfunction, microvascular and endothelial changes, viral persistence or residual viral material, reactivation of latent viruses, coagulation abnormalities, and tissue injury from the acute infection. In some individuals, symptom patterns overlap with conditions such as myalgic encephalomyelitis/chronic fatigue syndrome (ME/CFS), postural orthostatic tachycardia syndrome (POTS), mast cell-related symptoms, and post-intensive care syndromes.
From an integrative health perspective, Long COVID has drawn attention because recovery often involves more than one body system, and many patients seek strategies that support energy regulation, sleep quality, breathing, stress resilience, nutrition, and functional restoration. At the same time, experts emphasize that persistent symptoms warrant careful evaluation by qualified healthcare professionals, since ongoing issues such as cardiopulmonary disease, blood clotting complications, anemia, thyroid disease, or other treatable conditions may mimic or coexist with Long COVID.
Medical Perspectives
Two Ways of Seeing Health

Western
scientific · clinical
Western medicine applies science, technology, and clinical experience to treat symptoms through testing, diagnosis, and targeted intervention.

Eastern
traditional · alternative
Eastern medicine focuses on treating the body naturally by applying traditional knowledge practiced for thousands of years, emphasizing balance and whole-person wellness.
Gold Bamboo presents both perspectives side-by-side so you can make informed decisions. We don't advocate for one over the other — your health choices are yours.
Western Medicine Perspective
Western Medicine Perspective
In conventional medicine, Long COVID is approached as a multisystem post-infectious condition that requires individualized assessment rather than a single standard pathway. Clinical evaluation typically focuses on identifying symptom patterns, ruling out alternative explanations, and recognizing subtypes such as post-exertional symptom exacerbation, dysautonomia/orthostatic intolerance, respiratory limitations, neurocognitive symptoms, sleep disturbance, and mood-related effects. Because symptoms are varied and objective testing may be normal in some patients, contemporary care often emphasizes a combination of history, targeted testing, functional assessment, and symptom-informed rehabilitation.
Research indicates that management is still evolving. Conventional approaches may include pulmonary rehabilitation principles, autonomic support strategies, cognitive and occupational rehabilitation, sleep assessment, mental health support, and evaluation of cardiovascular or thrombotic risk where indicated. Importantly, clinicians increasingly recognize that some individuals experience post-exertional worsening, meaning aggressive exercise-based rehabilitation may not be appropriate for everyone. Instead, pacing-based approaches and careful energy management have become important considerations in many clinical settings.
Evidence for specific drug therapies remains limited, and no single medication is universally established for Long COVID. Investigational work is exploring anti-inflammatory, antiviral, anticoagulant, autonomic, and immunomodulatory approaches, but findings remain preliminary for many interventions. As a result, major institutions such as the CDC, WHO, NIH, and NICE generally frame current care around assessment, symptom management, functional support, and multidisciplinary follow-up, while research continues to clarify mechanisms and effective treatments.
Eastern & Traditional Perspective
Eastern/Traditional Medicine Perspective
In Traditional Chinese Medicine (TCM), persistent post-viral symptoms are often interpreted through patterns of qi deficiency, lung-spleen weakness, residual pathogenic factors, phlegm accumulation, blood stasis, or disruption of the shen depending on the symptom picture. For example, fatigue and poor stamina may be viewed through a deficiency pattern, while chest oppression, cognitive heaviness, or lingering cough may be described in terms of phlegm, dampness, or impaired lung function. TCM literature and contemporary integrative clinics have described the traditional use of acupuncture, breathing practices, dietary therapy, and individualized herbal formulations to support recovery, though high-quality evidence specific to Long COVID remains limited.
In Ayurveda, prolonged post-infectious symptoms may be conceptualized in relation to agni (digestive/metabolic function), ojas (vital resilience), and imbalances in doshas, particularly where fatigue, brain fog, disturbed sleep, and respiratory weakness predominate. Traditional frameworks may emphasize restoring overall vitality, supporting digestion and tissue recovery, and reducing lingering imbalance after illness. Naturopathic and other traditional systems similarly tend to focus on the terrain of recovery—sleep, stress physiology, nourishment, breath, gentle restoration, and individualized constitutional assessment.
From an evidence-based integrative standpoint, these systems may offer supportive frameworks for symptom relief and quality of life, especially where conventional care is largely symptomatic. However, the research base is still developing, and product quality, herb-drug interactions, and patient-specific risks remain important considerations. For that reason, traditional therapies are best understood as adjunctive approaches within coordinated care, particularly for people with cardiopulmonary symptoms, dysautonomia, clotting concerns, or complex medical histories.
Supplements & Products
Recommended Products

The Long Covid Handbook eBook : Medinger, Gez, Altmann, Professor Danny
This book is <strong>the definitive guide to understanding, managing and treating the condition</strong>. Written by the world's leading immunologist Professor Danny Altmann and expert patient Ge

NOW Foods Supplements, Ubiquinol 100 mg, High Bioavailability (the Active Form of CoQ10), 60 Softgels
Active Form of CoQ10 Highly Bioavailable <strong>Ubiquinol is the reduced and active free radical quencher form of coenzyme Q10 (CoQ10)</strong>.* CoQ10 is found in all cells of the body, with especia
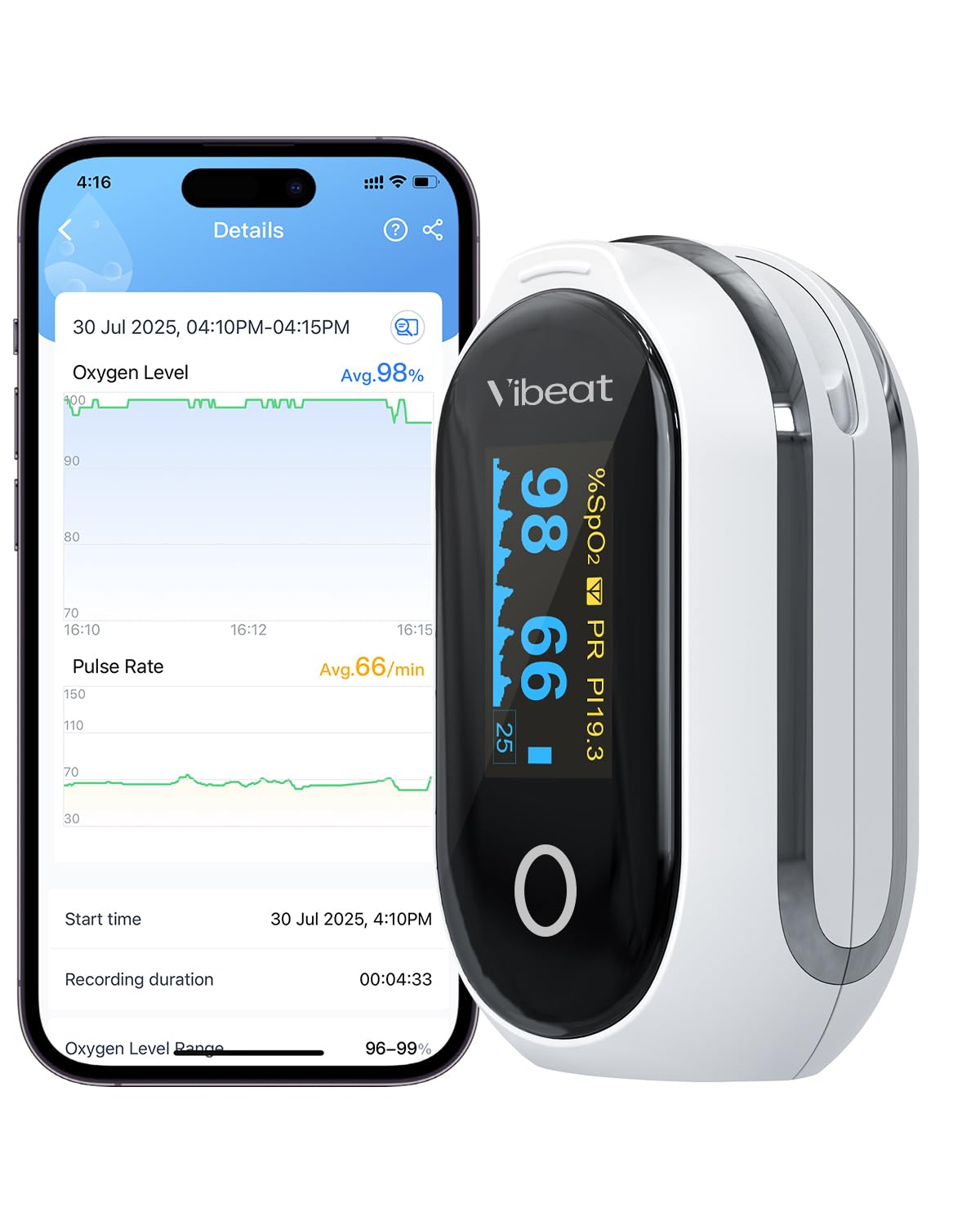
Masimo MightySat Fingertip Pulse Oximeter with Bluetooth ...
Monitor your blood oxygen levels and pulse with a <strong>compact, medical-grade pulse oximeter</strong>. Portable design with one-button operation and lanyard included.
Evidence & Sources
Promising research with growing clinical support from multiple studies
- World Health Organization (WHO)
- Centers for Disease Control and Prevention (CDC)
- National Institutes of Health (NIH) RECOVER Initiative
- National Institute for Health and Care Excellence (NICE)
- Nature Reviews Microbiology
- The Lancet
- JAMA
- BMJ
- National Center for Complementary and Integrative Health (NCCIH)
This content is for informational purposes only and does not constitute medical advice. Always consult a qualified healthcare provider before starting, stopping, or changing any supplement or medication regimen.

